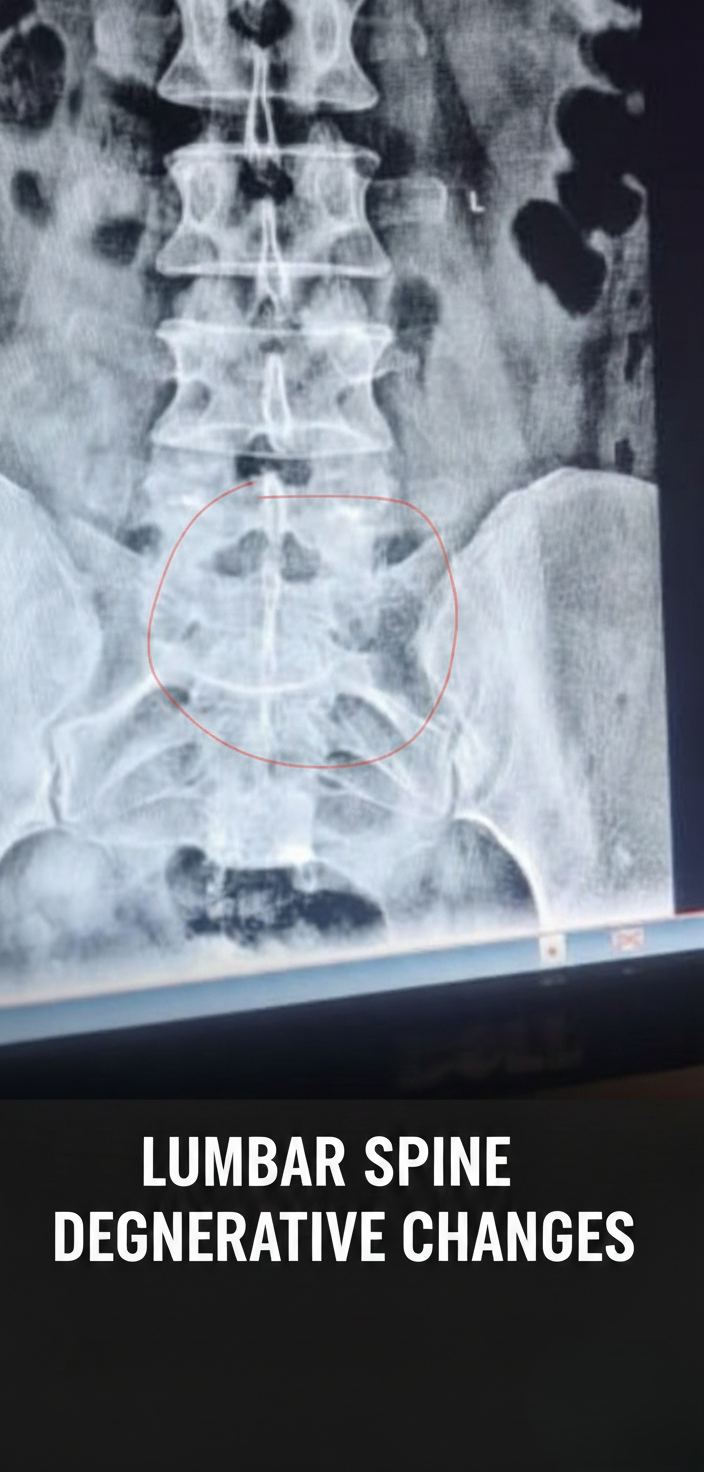
Degenerative Disc and Joint Disease (Osteoarthritis) of the Lumbar Spine
Degenerative disc and joint disease—commonly referred to as lumbar spine osteoarthritis (OA)—is a frequent contributor to persistent low back pain. It involves age- and load-related changes affecting the intervertebral discs and, importantly, the lumbar facet (zygapophyseal) joints, which play a key role in spinal stability and movement.
Lumbar OA develops through a combination of biomechanical stress and biological aging:
- Cartilage degeneration within facet joints leading to joint space narrowing and inflammation
- Disc degeneration (loss of hydration and height) increasing load transfer to facet joints
- Repetitive loading (prolonged sitting, heavy lifting, poor movement mechanics)
- Prior injury that accelerates degenerative change
- Lifestyle and metabolic factors (physical inactivity, obesity)
- Genetic factors
Common Symptoms
Symptoms vary widely and may fluctuate over time. Typical features include:
- Localized low back pain (often mechanical in nature)
- Pain aggravated by extension, prolonged standing, or sitting
- Morning stiffness
- Reduced lumbar mobility/ranges of motions
- Referred pain to the hips or buttocks (without true nerve root signs)
Neurological symptoms such as numbness or weakness in the lower extremities may suggest nerve involvement and require further evaluation.
Diagnosis
- Clinical: symptoms, age, and family history
- X-ray: disc space narrowing, osteophytes, facet joint sclerosis
- MRI: disc degeneration, facet joint arthropathy, synovial inflammation, neural involvement
- CT: detailed assessment of bony changes when needed
Imaging findings do not always correlate with symptoms.
- Some individuals show moderate or advanced degeneration with little or no pain
- Others may have mild degenerative changes but significant symptoms
This is often referred to as symptomatic osteoarthritis, where pain reflects joint irritation, inflammation, and nervous system sensitivity rather than the degree of structural change alone. Clinical correlation is essential, as emphasized in the BMJ Best Practice and the literature on spine OA.
Treatment and Care Plan
There is no cure for lumbar spine OA, but symptoms are commonly managed successfully with conservative, evidence-based care.
First-Line (Conservative) Management
- Patient education and reassurance
- Activity modification (avoid prolonged static positions)
- Exercise therapy: mobility, strengthening, aerobic conditioning
- Manual therapy where appropriate
- Lifestyle strategies (weight management, physical activity)
Symptom-Focused Management
- Short-term use of analgesics or anti-inflammatory medications (as advised by a physician)
- Structured rehabilitation during flare-ups
- Collaboration among chiropractors, physiotherapists, physicians, and specialists when required
In summary : Lumbar degenerative disc and joint disease is common and often manageable. Structural changes on imaging do not automatically explain pain. A diagnosis of symptomatic OA requires thoughtful clinical correlation. Evidence supports a conservative, movement-based, and patient-centered care plan as the foundation of management.
References:
BMJ Best Practice. (2024, November 20). Osteoarthritis. BMJ Publishing Group. https://bestpractice.bmj.com/topics/en-us/192
Kalichman, L., & Hunter, D. J. (2007). Lumbar facet joint osteoarthritis: A review. Seminars in Arthritis and Rheumatism, 37(2), 69–80. https://pubmed.ncbi.nlm.nih.gov/17379279/
Baroncini, A., et al. (2021). Management of facet joints osteoarthritis associated with chronic low back pain: A systematic review. Pain Physician. https://pubmed.ncbi.nlm.nih.gov/33582054/
Gellhorn, A. C., & Katz, J. N. (2013). Osteoarthritis of the spine: The facet joints. Nature Reviews Rheumatology. https://pubmed.ncbi.nlm.nih.gov/23147891/
Canadian Chiropractic Association. (2018). Recommended plan of management for low back pain (LBP) [PDF]. https://www.chiropractic.ca/wp-content/uploads/2018/04/CCGI-LBP-Recommended-Plan-Management-FINAL.pdf
Disclaimer
This content is intended for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Please always consult a qualified healthcare professional for individual assessment, diagnosis, or care.